You spend your entire life on your feet, and that pressure can wear on the cushioning that protects the bones in your feet from the ground you stand on. As you age, your body’s natural fat on the bottom of the foot is lost. This is called fat pad atrophy, and it is common in both men and women.
Fat pad atrophy can cause pain on the ball of the foot while you are walking. This is the common cause of discomfort that drives women away from wearing high heels or walking barefoot. Many people attempt to correct the issue by wearing highly cushioned insoles. However, these insoles are often not practical, as they limit footwear choices and do not eliminate the pain while barefoot.
Doctors at Palm Beach Foot & Ankle offer fat pad restoration in Boynton Beach, Palm Beach Gardens, and West Palm Beach so that you can walk freely and comfortably again.
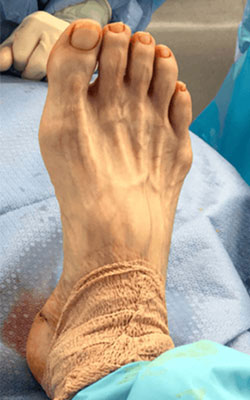 Before Treatment
Before Treatment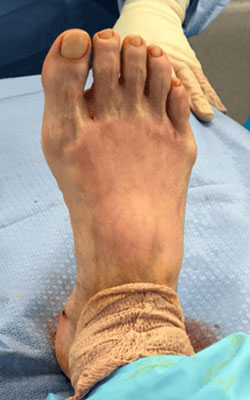 After Treatment
After TreatmentCauses of Fat Pad Atrophy
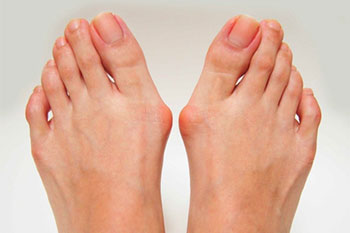
There are a number of conditions that can accelerate the breakdown of fat pads on the bottom of your feet. When these conditions develop, fat pad atrophy can occur as well. Sometimes, fat pad restoration can aid in the treatment of other foot conditions by enhancing comfort and restoring your ability to move.
Conditions that can sometimes be treated with fillers and fat pad restoration:
- Bunions
- Hammer toes
- Corns
- Calluses
- Diabetic ulcerations
- Neuropathy
- Plantar fasciitis
- Heel pad injections
- Cortisone injections
- Neuroma’s
- Metatarsalgia
- Bone Friction
- Smoking
Fat Pad Atrophy Symptoms
- Burning in the ball of the foot.
- Feeling like you are walking on pebbles.
- Bunched up sock feeling under your toes.
- Pounding feeling.
- Pressure sores.
Atrophy of the fat cushion on the bottom of the ball of the foot or the heel is a common condition. In the heel, there is an atrophy of the thickness of the fat cushion and is seen with plantar fasciitis. It may be mistaken for plantar fasciitis and your podiatrist in our Boynton Beach, Palm Beach Gardens, and West Palm Beach offices can tell the difference. If you have cortisone or steroid injections and the pain is not going away, consider a consultation and fat pad atrophy treatment. There is a loss of shock absorption when you step on the heel.
In the ball of the foot, there is that pad atrophy, or the fat moves under the toes and gives a bunched-up sock feeling in shoes. This is seen in people who have a high arch foot. This leads to pain and burning sensations. People often get calluses or corns and areas of skin irritation. The pain makes it difficult to perform activities we like to perform and wear shoes we like to wear.
Finally, on the top of the foot, you can develop loss of soft tissue, fat causing thin skin and you can see the tendons under the skin.
Fat Pad Restoration & Treatments
Fat pad restoration or enhancement of the fat on the bottom of the foot can be broken down into three categories.
- In-office Injectables
- Surgical Graft
- Fat Transfer otherwise known as Autolipotransplantation
In Office Injectables
Injectable fillers have been used for over 20 years. They are used in dermatology and plastic surgery and are now often used in the foot. This is performed in the office with little downtime and is a quick fix for foot pain that can keep you out of surgery. Whether you want to wear high heels, walk barefoot, or exercise, this treatment is a great option performed by our doctors in Boynton Beach, Palm Beach Gardens, and West Palm Beach. Currently, we used RadiesseR, SculptraR, and Juvederm VolumaR. Walk-in with pain and walk-out more cushioned! The injections work great on high-pressure areas causing corns and calluses.
LenevaR Is the newest treatment and the first of its kind injectable fat graft used for fat pad restoration. It is an Adipose Allograft Matrix (AAM) which is a graft that when placed into the foot works to build fat tissue over the course of twelve weeks. The graft is safe to use has been shown to provide new soft tissue thickness and has improved the quality of skin conditions such as corns, calluses, and skin ulceration as seen in diabetics or neuropathy patients.
During your visit, if the treatment is right for you, it is performed in the office. The doctor will obtain x-rays, and perform an ultrasound to look at the area to be treated. The ultrasound is helpful to identify the extent of fat pad atrophy and show the exact location to perform the injection. Numbing medication is used on the skin and the injection is painless! The doctors do not use a needle, but use a blunt tip injector to insert the medication into the foot. Adhesive pads are placed on the foot and light pressure with walking is allowed immediately. You will be provided with complete instructions for post-procedure care. It is recommended that minimal exercise is performed for at least one week after the procedure. In more severe cases, the doctor may provide a special shoe during your healing process.
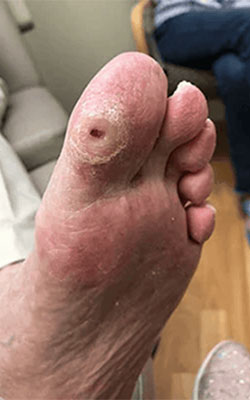
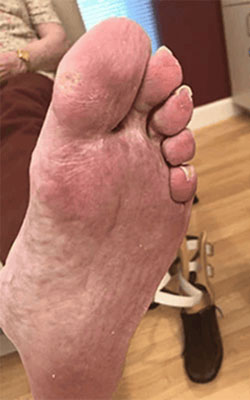
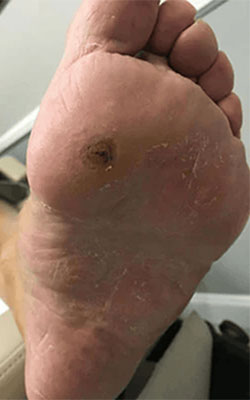
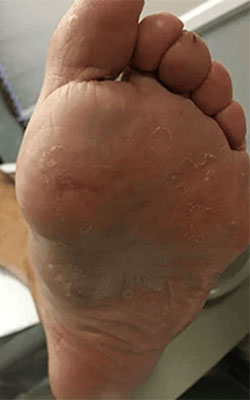

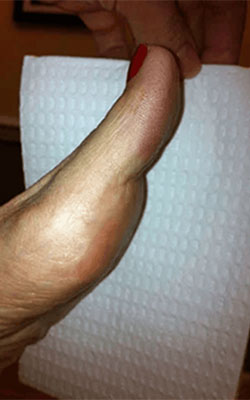
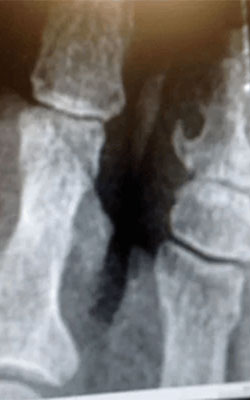
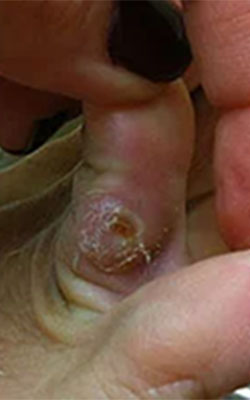
Fat Pad Surgery
If surgery is needed for other conditions such as a bunion, we will often use a graft and place it into the foot. This is a layered cushion of tissue that is placed under the skin and provides an extra layer of padding. It is anchored with a skin suture and becomes incorporated into your tissue within a few weeks. It is recommended to remain off of the foot for approximately one week after treatment.
Fat Pad Transfer
Fat transfer or Autolipotransplantation is another fat pad cushioning procedure. We work with our team of plastic surgeons to take your own fat from the stomach or buttocks and it is placed into the foot. This procedure can be formed in the office or in an outpatient surgical suite. There is a slightly longer recovery time with the procedure due to the liposuction site and the foot healing, however, you can walk with a special shoe immediately after the procedure. We have found this procedure lasts the longest and touch ups can be injected at a later date. On occasion, we will mix the fat with amnion stem cell or PRP (protein rich plasma) to stimulate the fat and lay down more padding tissue. This procedure is often used when larger volumes of fat are needed in the foot. By transferring fat from one body part to another, we can cushion the bones of the foot and provide a more comfortable pillow to walk on.
These techniques offer patients foot pad pain relief and allows them improvement in comfort and shoes as well as activity and utility to even walk barefoot.
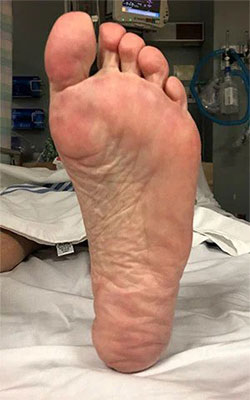 Before Treatment
Before TreatmentFat Pad Transfer to the Ball of the Foot
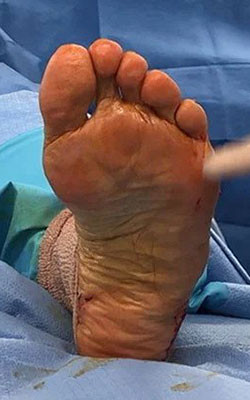 After Treatment
After TreatmentFat Pad Transfer to the Ball of the Foot
